States are making tepid progress helping millions of elderly and disabled people on Medicaid avoid costly nursing home care by arranging home or community services for them instead, according to an AARP report released Wednesday.
“Although most states have experienced modest improvements over time, the pace of change is not keeping up with demographic demands,” said the report, which compared states’ efforts to improve long-term care services over the past several years. AARP’s first two reports on the subject were in 2011 and 2014.
The organization ranked states’ performance on long-term care benchmarks such as supply of home health aides, nursing home costs, long nursing home stays, the employment rate of people with disabilities and support for working caregivers.
California ranked ninth overall in 2014, up from 15th 2011.
With 10,000 people a day turning 65 and the eldest baby boomers beginning to turn 80 in 2026, the demand for long-term care services is expected to soar in coming years.
AARP officials said the House’s bill to repeal the Affordable Care Act would worsen the situation by capping annual federal revenue for states’ Medicaid programs. That bill is now before the Senate.
“The proposed cuts to Medicaid — the largest public payer of long-term assistance — would result in millions of older adults and people with disabilities losing lifesaving supports,” said Susan Reinhard, senior vice president and director of the AARP Public Policy Institute.
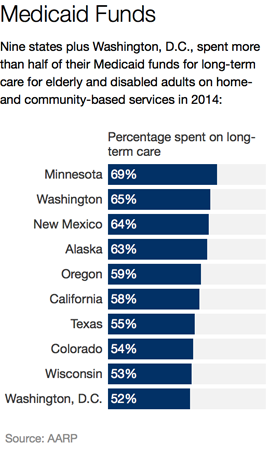
The report found strikingly wide variances in the share of state Medicaid spending for long-term care directed to home- and community-based services for elderly and disabled adults in 2014, the latest year for data covering all states.
Only nine states and the District of Columbia spent more of their long-term care Medicaid dollars on home- and community-based services than on nursing home care, according to the report. Such services include home health care, caregiver training and adult day care.
Minnesota, the top-ranked state, spent about 69 percent of its long-term care money on home- and community-based services, but Alabama, ranked last, spent less than 14 percent. California spent about 58 percent, earning it the ranking of sixth in the nation.
Nationwide, the average edged up from 39 percent in 2011 to 41 percent in 2014.
“There are lots of problems with long-term services and supports under Medicaid, but states are really making progress,” said H. Stephen Kaye, a professor at the Institute for Health & Aging at the University of California, San Francisco.
Kaye agreed that the proposed House health bill would seriously compromise the gains that have been made in California and around the nation. He said that if the bill passed, he could foresee future scorecards showing little improvement.
“Home and community-based services really do work, and they really do keep people out of nursing homes,” he said. But if Medicaid funding caps were in place, Kaye said, that “would really discourage states, especially the laggard states, from doing anything new or forward thinking.”
The report also ranked states based on several other factors, including affordability of home care and how much choice people had in where they received care. California ranked 19th for affordability and third for providing choice of setting. That’s partly because of the state’s In-Home Supportive Services program, which allows Medicaid recipients to directly hire home caregivers.
In addition, the state ranked eighth for support of family caregivers. California and a handful of other states have legislation allowing residents to take time off work to take care of family members.
People turning 65 this year face about a 50-50 chance of needing long-term care services in their lifetime, AARP officials said.
Trish Riley, executive director of the National Academy for State Health Policy, said states face several obstacles to expand home- and community-based options. They include a strong nursing home lobby that does not want to give up its Medicaid dollars and a shortage of transportation and housing options, particularly in rural areas.
An Alabama Medicaid spokeswoman said the state is working on the issue highlighted by AARP but refused to comment on its report.
 John Matson, a spokesman for the Alabama Nursing Home Association, rejected the notion that nursing homes are to blame. “We think it’s a shift that needs to happen in Alabama. … We can’t build enough nursing homes to meet [the needs of] everyone that is coming,” he said.
John Matson, a spokesman for the Alabama Nursing Home Association, rejected the notion that nursing homes are to blame. “We think it’s a shift that needs to happen in Alabama. … We can’t build enough nursing homes to meet [the needs of] everyone that is coming,” he said.
The state’s effort to shift Medicaid patients from long-term care into managed care organizations starting next year will help, because those entities will have a financial incentive to keep people at home for care when possible, Matson said.
Reinhard said many states have struggled to expand home- and community-based options for Medicaid enrollees needing long-term care because that is an optional benefit. Nursing homes are mandatory under federal law. While states focus on Medicaid coverage for children and families — as well as non-disabled adults covered by the Medicaid expansion under the Affordable Care Act — adults with disabilities have received less attention.
“Long-term care is a stepchild of the program and not a top focus for states,” she said.
To view the full report, go to www.longtermscorecard.org. The report was funded by the AARP Foundation, The Commonwealth Fund and The SCAN Foundation. (Kaiser Health News, which produces California Healthline, is supported in part by a grant from The SCAN Foundation for coverage of aging and long-term care issues .)
Kaiser Health News reporter Anna Gorman contributed to this story.
This story was produced by Kaiser Health News, an editorially independent program of the Kaiser Family Foundation.


