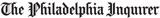PHILADELPHIA — Carol Emanuele beat cancer. But for the past two years, she has been fighting her toughest battle yet. She has an open wound on the bottom of her foot that leaves her unable to walk and prone to deadly infection.
In an effort to treat her diabetic wound, doctors at a Philadelphia clinic have prescribed a dizzying array of treatments. Freeze-dried placenta. Penis foreskin cells. High doses of pressurized oxygen. And those are just a few of the treatment options patients face.
“I do everything, but nothing seems to work,” said Emanuele, 59, who survived stage 4 melanoma in her 30s. “I beat cancer, but this is worse.”
The doctors who care for the 6.5 million patients with chronic wounds know the depths of their struggles. Their open, festering wounds don’t heal for months and sometimes years, leaving bare bones and tendons that evoke disgust even among their closest relatives.
Many patients end up immobilized, unable to work and dependent on Medicare and Medicaid. In their quest to heal, they turn to expensive and sometimes painful procedures, and products that often don’t work.
According to some estimates, Medicare alone spends at least $25 billion a year treating these wounds. But many widely used treatments aren’t supported by credible research. The $5 billion-a-year wound care business booms while some products might prove little more effective than the proverbial snake oil. The vast majority of the studies are funded or conducted by companies who manufacture these products. At the same time, independent academic research is scant for a growing problem.
“It’s an amazingly crappy area in terms of the quality of research,” said Sean Tunis, who as chief medical officer for Medicare from 2002 to 2005 grappled with coverage decisions on wound care. “I don’t think they have anything that involves singing to wounds, but it wouldn’t shock me.”
A 2016 review of treatment for diabetic foot ulcers found “few published studies were of high quality, and the majority were susceptible to bias.” The review team included William Jeffcoate, a professor with the Department of Diabetes and Endocrinology at Nottingham University Hospitals Trust. Jeffcoate has overseen several reviews of the same treatment since 2006 and concluded that “the evidence to support many of the therapies that are in routine use is poor.”
“I don’t think they have [any therapy] that involves singing to wounds, but it wouldn’t shock me.”
A separate Health and Human Services review of 10,000 studies examining treatment of leg wounds known as venous ulcers found that only 60 of them met basic scientific standards. Of the 60, most were so shoddy that their results were unreliable.
While scientists struggle to come up with treatments that are more effective, patients with chronic wounds are dying.
The five-year mortality rate for patients with some types of diabetic wounds is more than 50 percent higher than breast and colon cancers, according to an analysis led by Dr. David Armstrong, a professor of surgery and director of the Southern Arizona Limb Salvage Alliance.
Open wounds are a particular problem for people with diabetes because a small cut may turn into an open crater that grows despite conservative treatment, such as removal of dead tissue to stimulate new cell growth.
More than half of diabetic ulcers become infected, 20 percent lead to amputation, and, according to Armstrong, about 40 percent of patients with diabetic foot ulcers have a recurrence within one year after healing.

Carol Emanuele of Philadelphia shows a photograph of a wound VAC (vacuum-assisted closure) procedure on her left foot after the amputation of her big toe. (Eileen Blass/for Kaiser Health News)
“It’s true that we may be paying for treatments that don’t work,” said Tunis, now CEO of the nonprofit Center for Medical Technology Policy, which has worked with the federal government to improve research. “But it’s just as tragic that we could be missing out on treatments that do work by failing to conduct adequate clinical studies.”
Although doctors and researchers have been calling on the federal government to step in for at least a decade, the National Institutes of Health and the Veterans Affairs and Defense departments haven’t responded with any significant research initiative.
“The bottom line is that there is no pink ribbon to raise awareness for festering, foul-smelling wounds that don’t heal,” said Caroline Fife, a wound care doctor in Texas. “No movie star wants to be the poster child for this, and the patients … are old, sick, paralyzed and, in many cases, malnourished.”
The NIH estimates that it invests more than $32 billion a year in medical research. But an independent review estimated it spends 0.1 percent studying wound treatment. That’s about the same amount of money NIH spends on Lyme disease, even though the tick-borne infection costs the medical system one-tenth of what wound care does, according to an analysis led by Dr. Robert Kirsner, chair and Harvey Blank professor at the University of Miami Department of Dermatology and Cutaneous Surgery.
Emma Wojtowicz, an NIH spokeswoman, said the agency supports chronic wound care, but she said she couldn’t specify how much money is spent on research because it’s not a separate funding category.
“Chronic wounds don’t fit neatly into any funding categories,” said Jonathan Zenilman, chief of the division for infectious diseases at Johns Hopkins Bayview Medical Center and a member of the team that analyzed the 10,000 studies. “The other problem is it’s completely unsexy. It’s not appreciated as a major and growing health care problem that needs immediate attention, even though it is.”
Commercial manufacturers have stepped in with products that the FDA permits to come to market without the same rigorous clinical evidence as pharmaceuticals. The companies have little incentive to perform useful comparative studies.
“There are hundreds and hundreds of these products, but no one knows which is best,” said Robert Califf, who stepped down as Food and Drug Administration commissioner for the Obama administration in January. “You can freeze it, you can warm it, you can ultrasound it, and [Medicare] pays for all of this.”
When Medicare resisted coverage for a treatment known as electrical stimulation, Medicare beneficiaries sued, and the agency changed course.
“The ruling forced Medicare to reverse its decision based on the fact that the evidence was no crappier than other stuff we were paying for,” said Tunis, the former Medicare official.
In another case, Medicare decided to cover a method called “noncontact normothermic wound therapy,” despite concerns that it wasn’t any more effective than traditional treatment, Tunis said.
“It’s basically like a Dixie cup you put over a wound so people won’t mess with it,” he said. “It was one of those ‘magically effective’ treatments in whatever studies were done at the time, but it never ended up being part of a good-quality, well-designed study.”
The companies that sell the products and academic researchers themselves disagree over the methodology and the merits of existing scientific research.
Thomas Serena, one of the most prolific researchers of wound-healing products, said he tries to pick the healthiest patients for inclusion in studies, limiting him to a pool of about 10 percent of his patient population.
“We design it so everyone in the trial has a good chance of healing,” he said.
“If it works, like, 80 or 90 percent of the time, that’s because I pick those patients,” said Serena, who has received funding from manufacturers.
But critics say the approach makes it more difficult to know what works on the sickest patients in need of the most help.
Gerald Lazarus, a dermatologist who led the HHS review as then-director of Johns Hopkins Bayview Medical Center wound care clinic, said Serena’s assertion is “misleading. That’s not a legitimate way to conduct research.” He added that singling out only healthy patients skews the results.
The emphasis on healthier patients in clinical trials also creates unrealistic expectations for insurers, said Fife.
“The expensive products … brought to market are then not covered by payers for use in sick patients, based on the irrefutable but Kafka-esque logic that we don’t know if they work in sick people,” she said.
“Among very sick patients in the real world, it may be hard to find a product that’s clearly superior to the others in terms of its effectiveness, but we will probably never find that out since we will never get the funding to analyze the data,” added Fife, who has struggled to get government funding for a nonprofit wound registry she heads. Not surprisingly, she said, the registry data demonstrate that most treatments don’t work as well on patients as shown in clinical trials.
Patients say they often feel overwhelmed when confronted with countless treatments.
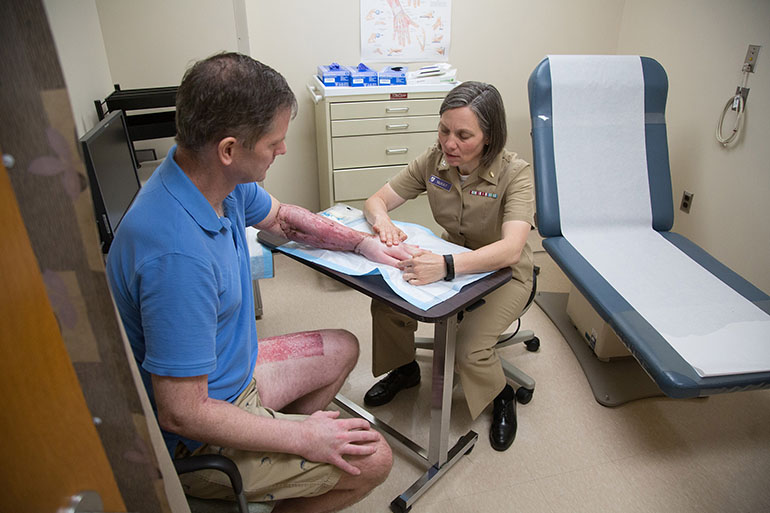
Navy surgeon Capt. Pat McKay examines the healing progress of skin grafts on Navy Cmdr. Peter Snyder at Walter Reed National Military Medical Center. (H. Darr Beiser/for Kaiser Health News)
“Even though I’m a doctor and my wife is a nurse, we found this to be complicated,” said Navy Cmdr. Peter Snyder, a radiologist who is recovering from necrotizing fasciitis, also known as flesh-eating bacteria. “I can’t imagine how regular patients handle this. I think it would be devastating.”
To heal wounds on his arms and foot, Snyder relied on various treatments, including skin-graft surgery, special collagen bandages and a honey-based product. His doctor who treats him at Walter Reed National Military Medical Center predicted he would fully recover.
Such treatments aren’t always successful. Although Emanuele’s wound left by an amputation (of her big toe) healed, another wound on the bottom of her foot has not.
Recently, she looked back at her calendar and marveled at the dozens of treatments she has received, many covered by Medicare and Medicaid.

To help Carol Emanuele get around her Philadelphia home, she places a walker inside the threshold of the doorway to her bathroom so she can easily transfer from wheelchair or a walker in order to stay off her feet. (Eileen Blass/for Kaiser Health News)
Some seem promising, like wound coverings made of freeze-dried placenta obtained during births by cesarean section. Others, not — including one plastic bandage that her nurse agreed made her wound worse.
Emanuele was told she needed to undergo high doses of oxygen in a hyperbaric chamber, a high-cost treatment hospitals are increasingly relying on for diabetic wounds. The total cost: about $30,000, according to a Medicare invoice.
Some research has indicated that hyperbaric therapy works, but last year a major study concluded it wasn’t any more effective than traditional treatment.
“Don’t get me wrong, I am grateful for the care I get,” Emanuele said. “It’s just that sometimes I’m not sure they know what they’re using on me works. I feel like a guinea pig.”
Confined to a wheelchair because of her wounds, she fell moving from the bathroom to her wheelchair and banged her leg, interrupting the healing process. Days later, she was hospitalized again. This time, she got a blood infection from bacteria entering through an ulcer.
She has since recovered and is now back on the wound care routine at her house.
“I don’t want to live like this forever,” she said. “Sometimes I feel like I have I no identity. I have become my wound.”
This story was produced by Kaiser Health News, an editorially independent program of the Kaiser Family Foundation.