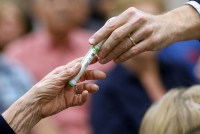
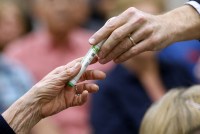
¿Como la diabetes? Legisladores buscan nuevas formas de tratar adicción a opioides
Un proyecto de ley requeriría que las aseguradoras privadas cubrieran los medicamentos para la adicción a los opioides sin necesidad de aprobación previa.
As Treatable As Diabetes? Lawmakers Push New Ways To Stem Opioid Addiction
California lawmakers approved 14 measures to address the opioid crisis, including one that requires health plans to cover medication-based treatments for opioid addiction without requiring pre-authorization. Gov. Jerry Brown has until the end of September to approve or reject the proposals.
From Stethoscope To Gavel: Pediatrician At Center Of State’s Health Care Debates
State Sen. Richard Pan, a pediatrician who still sees patients once a week, is the new chairman of the Senate Health Committee. He takes this leadership role as he seeks re-election and as the state is battling federal cuts and preparing for a new governor.
Shortage Of Insurance Fraud Cops Sparks Campaign Debate
About a quarter of fraud investigator positions at the state Department of Insurance are open, and Steve Poizner has made the vacancies a focus of his campaign for insurance commissioner. His opponent, Ricardo Lara, says chasing criminals isn’t the only solution to rising health care costs.
Medicaid Expansion Making Diabetes Meds More Accessible To Poor, Study Shows
The number of diabetes drug prescriptions filled for low-income people enrolled in Medicaid rose sharply in states that expanded eligibility for the program under the Affordable Care Act, according to a new study.
Expansión de Medicaid facilita el acceso de los más pobres a drogas anti diabetes
El estudio revela que las recetas para drogas contra la diabetes aumentaron un 40% en los estados que expandieron Medicaid bajo ACA. También lo hicieron los diagnósticos.
California’s ACA Rates To Rise 8.7% Next Year
The average increase in California is smaller than the double-digit hikes expected around the nation, due largely to a healthier mix of enrollees and more competition in its marketplace. Still, health insurance prices keep growing faster than wages and general inflation.
Doctors And Dentists Welcome Pay Hike For Treating Low-Income Patients
California is boosting rates for doctors and dentists who participate in the state’s Medi-Cal program for low-income residents. Providers say the pay raises will increase their participation in the program and improve access for patients.
California Poised To Expand Access To Hepatitis C Drugs
New state rules and funding, which are pending approval from the governor, would make almost all Medi-Cal recipients with hepatitis C eligible for pricey, lifesaving medications, as long as they are at least 13 and have more than one year to live.
New Hospital Leader Fights Price Controls Despite Reputation As A Reformer
Carmela Coyle was known as an innovator when she led Maryland’s hospital association and supported a groundbreaking program that capped hospital revenue. But less than a year into her new job representing California’s hospitals in Sacramento, Coyle has already helped kill a proposal to regulate pricing.