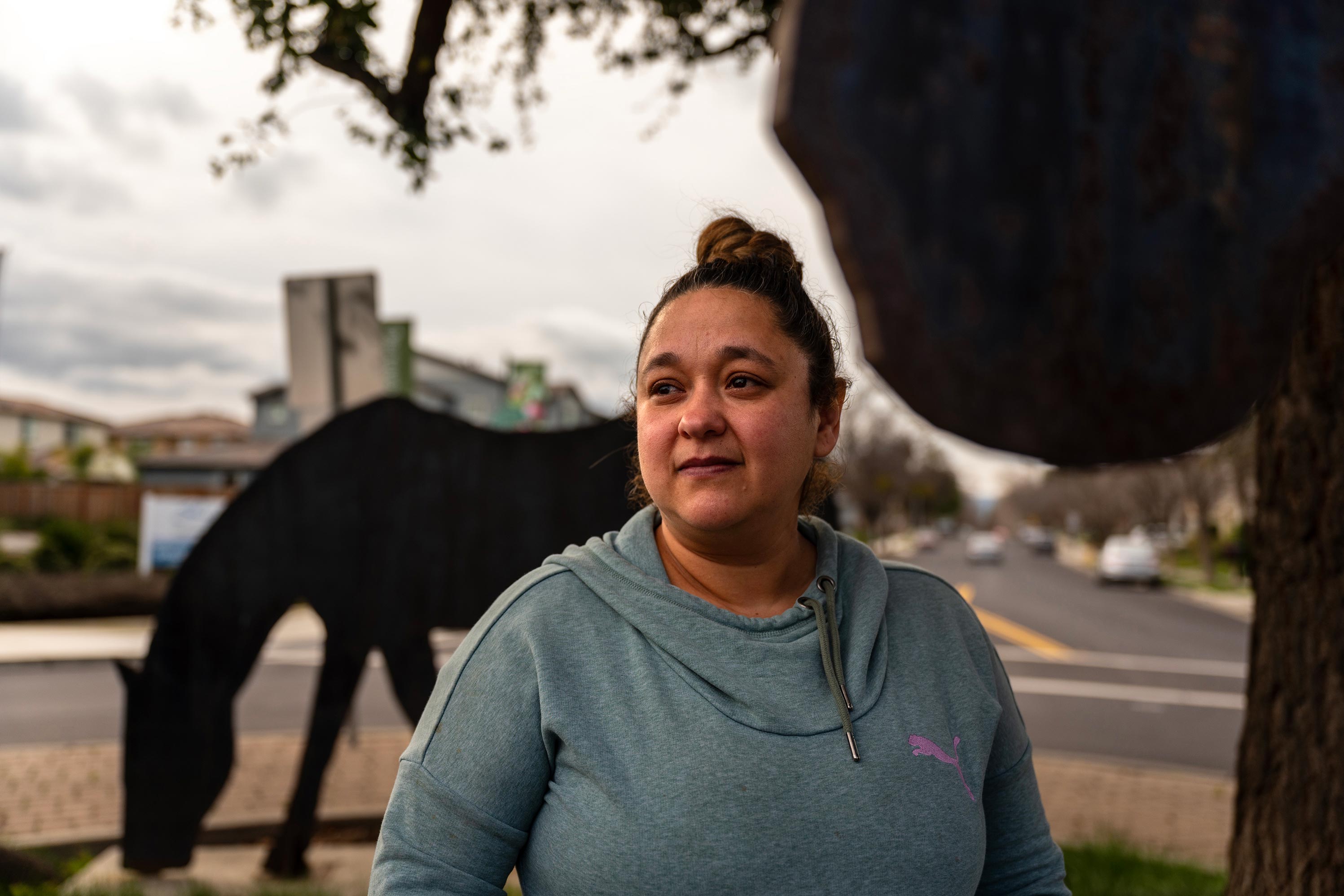Latest California Healthline Stories
Longtime Head of L.A. Care To Retire After Navigating Major Medi-Cal Changes
John Baackes, who steered Medi-Cal’s largest health plan following the Affordable Care Act expansion, and later prepared it for a state overhaul of Medi-Cal, will retire after this year. Baackes believes low payments to doctors and other providers, along with an acute labor shortage, hamper Medi-Cal’s success.
Medi-Cal’s Dental Care Gap: Getting a Tooth Pulled Is Easy — Much Harder To Get an Implant
California is among a growing number of states that offer dental benefits to low-income residents, but some lawmakers want the state to go further by covering more cleanings and costlier implants. Dentists and health experts worry the approach doesn’t address the root of the problem: Many providers don’t accept Medicaid.
California Leaders Tussle With Health Industry Over Billions of New Dollars for Medi-Cal
Gov. Gavin Newsom wants to pull funds earmarked for new investment in Medi-Cal to help plug California’s $45 billion deficit. A state budget passed June 13 by the legislature largely endorsed Newsom’s plan. Voters could settle the matter in an industry-backed initiative that has qualified for the November ballot.
California Lawmakers Preserve Aid to Older, Disabled Immigrants
Lawmakers passed a budget that rejected Gov. Gavin Newsom’s proposal to save nearly $95 million by eliminating in-home support services for qualifying older, blind, and disabled immigrants lacking legal residency. Advocates say Newsom’s plan would have cost more in the long run. Newsom has not indicated whether he’ll veto.
‘I Try To Stay Strong’: Mom Struggles To Get Diagnosis for Son’s Developmental Problems
An Alameda County mother has spent 10 months seeking help for her 4-year-old son’s speech and behavior issues from his school district and her Medicaid health insurer. She still doesn’t have an answer.
California Becomes Latest State To Try Capping Health Care Spending
California is the ninth state to set annual health spending targets for the industry. Already hospitals and doctors are voicing resistance to the fledgling Office of Health Care Affordability, even as they avoid overtly opposing its goals.
California Pays Meth Users To Get Sober
California’s Medicaid program is testing a novel approach for people addicted to methamphetamine, cocaine, and other stimulants. For every clean urine test, they can earn money — up to $599 a year.
Newsom’s $12 Billion Medicaid Makeover Banks on Nonprofits’ Buy-In
California’s Medicaid program is relying heavily on community groups to deliver new social services to vulnerable patients, such as security deposits for homeless people and air purifiers for asthma patients. But many of these nonprofits face staffing and billing challenges and haven’t been able to deliver services effectively.
California Floats Extending Health Insurance Subsidies to All Adult Immigrants
The legislature is considering taking the first steps to make Covered California plans available to immigrants without permanent legal status. The state has already extended Medi-Cal coverage to low-income immigrants.
California propone ampliar subsidios de seguros de salud a todos los inmigrantes adultos
California es el primer estado en ampliar Medicaid a todos los adultos que reúnan los requisitos, independientemente de su estatus migratorio, una medida celebrada por los activistas de la salud y por líderes políticos de todo el estado.